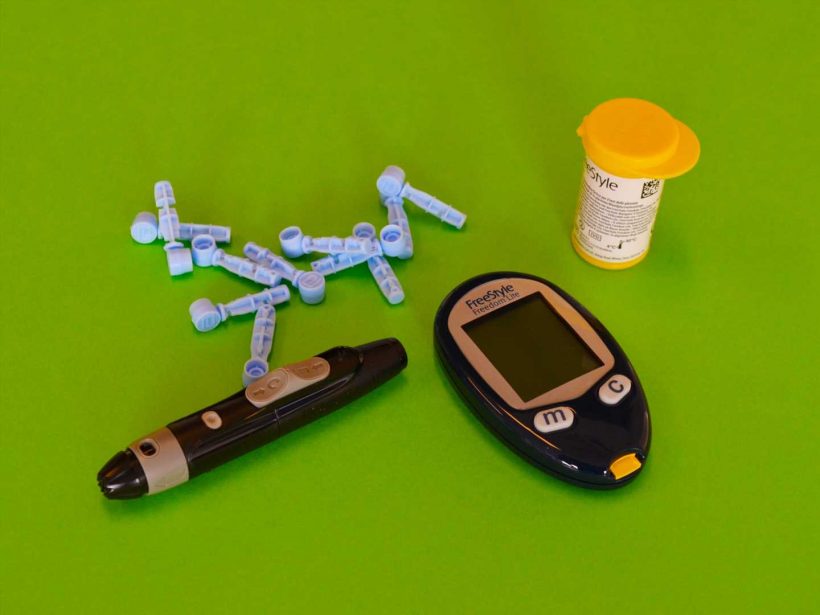
Monitoring the level of glucose (sugar) in your blood is vital if you have diabetes. You get results in real-time, which allows you to adjust your medications, exercise and food accordingly.
Because blood glucose levels fluctuate throughout the day, monitoring improves glucose control and reduces the risks of complications from hypoglycemia (low blood glucose) and hyperglycemia (high glucose levels).
But the type and range of blood glucose monitors has increased in recent years. Here are the two main options, with their pros and cons.
Finger prick tests
The first blood glucose monitors were the finger prick tests, which were developed over 50 years ago and are still in use today. These rely on you pricking your finger and placing a drop of blood on a strip, which you insert into a handheld meter.
Meters available in Australia must meet international standards for accuracy. There are many approved meters and strips subsidized under the National Diabetes Services Scheme.
If you have type 2 diabetes and need infrequent testing (mostly people who are not taking insulin) these devices may be suitable.
However, it can be unpleasant or impractical to prick your finger several times a day, especially if you require more frequent monitoring.
Continuous glucose monitoring
Continuous glucose monitoring has transformed glucose testing over the past 20 years or so, particularly for people who need insulin injections or use an insulin pump.
These systems use sensors you usually stick on to your arm or abdomen. The sensor has a tiny needle that pierces the skin to measure glucose levels under the skin (subcutaneous glucose) every few minutes. The reading is then transmitted to a device, such as a smartphone or receiver. These systems also need to meet international standards for accuracy.
Because the glucose level under the skin is not exactly the same as the blood glucose level, an algorithm transforms this into a blood glucose reading.
These systems provide real-time glucose information and have become increasingly accurate and user friendly over time. All have alarms to alert the wearer to dangerously low or high glucose levels. These alarms bring peace of mind to users and caregivers who fear the consequences of severe hypos, particularly during the night or during activities, such as driving.
But there is a time lag between subcutaneous glucose and blood glucose of a few minutes that means continuous monitoring is always running a bit behind.
Applying pressure to the sensor (for example, sleeping on it) can affect its accuracy, as can various medications or supplements such as vitamin C or paracetamol.
You also cannot use these devices straight away. There’s a one to two hour warm-up period after applying them to the skin.
Then there’s the cost. Since 2022, all people with type 1 diabetes have had subsidized access to continuous monitoring under the National Diabetes Services Scheme. But there is no such subsidy for people with type 2 diabetes, who have to pay around A$50 a week for their systems.
Other options
The sensors for the continuous monitoring systems last for one to two weeks, depending on the system; then you have to apply a new sensor. But there are implantable devices in development that will last six months. These are not yet available in Australia.
Other devices based on watches that are widely advertised are not approved glucose monitors. There is no scientific evidence supporting their accuracy.
Whichever device you use or are considering, it is important you do so with your treating medical practitioner, specialist or diabetes nurse educator.
Provided by
The Conversation
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Source: Read Full Article