Researchers at the University of São Paulo (USP) in Brazil have identified a new class of molecules capable of stopping the excessive inflammation typical of the severe form of COVID-19 without impairing the immune response to SARS-CoV-2, the virus that causes the disease.
The researchers conducted experiments with mice showing that the inflammation triggered by the cytokine storm was reduced when they blocked the link between a peptide called C5a and its cellular receptor, the protein C5aR. The study is reported in an article published in the Journal of Clinical Investigation (JCI).
“We’ve been studying this pathway for some years in connection with neuropathic pain and autoimmune disorders. When the pandemic began, we suspected that blocking the cellular receptor of this peptide [C5a] could also be a way of mitigating the inflammation associated with severe COVID-19, because it plays an important pro-inflammatory role but is dispensable for infection control. It’s a mediator, and blocking it doesn’t impair the immune response against the virus,” said Thiago Mattar Cunha, last author of the article.
Cunha is a professor at the Ribeirão Preto Medical School (FMRP-USP) and a researcher affiliated with the Center for Research on Inflammatory Diseases (CRID).
During the pandemic, it became obvious that COVID-19 could vary widely in terms of severity. While many patients had mild symptoms or none, a significant proportion suffered from potentially fatal inflammation triggered by an exacerbated immune response known as cytokine storm syndrome. These patients typically spent days in hospital intensive care units, required mechanical ventilation, and had complications such as pulmonary fibrosis and thrombosis.
As Cunha explained, C5 is an inflammatory mediator present in blood plasma and a component of the complement system, the part of the immune response responsible for forming the cascade of proteins that induces inflammation to combat an infection.
When the peptide is activated in response to infection, it becomes C5a and assumes a pro-inflammatory function. “The increase in production of C5a is associated with several inflammatory diseases, such as sepsis, rheumatoid arthritis, inflammatory bowel disease, lupus and psoriasis, and also with the lung damage seen in severe cases of COVID-19,” Cunha said.
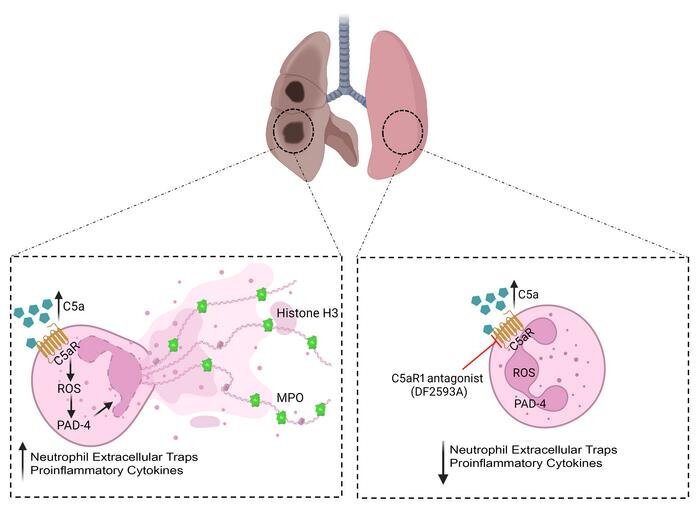
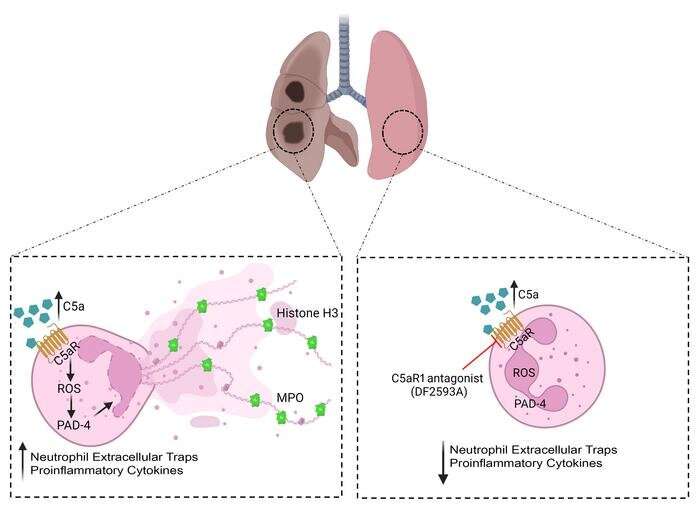
Previous research by CRID had already shown NETosis, a regulated form of cell death, to be one of the main ways COVID-19 patients suffer lung damage. Neutrophil extracellular traps (NETs), a part of the immune system, are networks of DNA strings released from neutrophils, a type of white blood cell, into the extracellular space during inflammation to defend against invading pathogens. NETosis is NET activation and release.
The researchers set out to elucidate the mechanism whereby C5 participates in the lung damage and exacerbated inflammation observed in severe COVID-19 patients. To do so, they used genetically modified (GM) mice susceptible to COVID-19 but with the gene that encodes for C5 knocked out.
According to Cunha, these animal model trials showed that NETs released in the lungs are harmful to the patient’s cells as well as the virus. “This pathway is not only involved in pulmonary epithelial cell death, as shown by one of our first studies on the topic, but also possibly associated with inflammation through thromboembolism in the lungs of COVID-19 patients,” he said.
The findings confirm the immunopathological role of the C5a/C5aR1 pathway in COVID-19 and indicate that antagonists of C5aR1 (molecules that prevent binding to the receptor) could be useful for treatment of severe COVID-19.
“Several processes are involved. C5 increases formation of NETs. Neutrophils are recruited to the lungs because cytokine production is intense in this stage of the disease, and C5a further boosts neutrophil activation in the lungs, leading to production of even more NETs. In light of all this, it’s likely that the pathway is involved in amplifying lung damage and inflammation,” Cunha said.
Before the pandemic, the CRID group was collaborating with Dompé, an Italian pharmaceutical company, to develop molecules that could block C5aR1. Some of their research findings were published in 2014 in Proceedings of the National Academy of Sciences.
“In our latest study, the inflammation improved in the mice that received C5aR1 antagonists. We also showed that infection control was not altered when this system was blocked: viral load was the same in the mice treated with the antagonists and those not treated,” Cunha said.
Improving inflammation without affecting viral load is an important property of the novel molecule. One of the main current strategies for treating COVID-19 is the use of corticoids, which are both anti-inflammatory and immunosuppressant. This class of drugs, therefore, reduces the immune response to SARS-CoV-2 as well as secondary infections, such as bacterial pneumonia, for example.
Although the CRID group has conducted experiments only on animals, Cunha recalled a study published late last year in The Lancet by European researchers on the benefits of blocking the C5a/C5aR1 pathway in humans. This paper described the results of Phase 3 clinical trials using a monoclonal antibody against C5a, showing that this is an effective strategy to combat exacerbated inflammation in COVID-19.
“When the antibody binds to C5a, it prevents action in the receptor. This means the clinical trials are working on the same pathway as the one our study focuses on and suggests we’re on the right track,” he said.
The advantage of the Brazilian strategy is that the cost of treatment with C5aR1 antagonists is much lower than the cost of treatment with monoclonal antibodies.
“The findings in this study provide clinical evidence that blocking the C5a/C5aR1 pathway works and is a beneficial treatment. In previous research, we focused on this pathway for autoimmune diseases and pain. I believe the next step is to start clinical trials with the antagonist molecule,” he said.
More information:
Bruna M. Silva et al, C5aR1 signaling triggers lung immunopathology in COVID-19 through neutrophil extracellular traps, Journal of Clinical Investigation (2023). DOI: 10.1172/JCI163105
Journal information:
Proceedings of the National Academy of Sciences
,
Journal of Clinical Investigation
,
The Lancet
Source: Read Full Article