A blood-based tumor biomarker can predict the benefit of immunotherapy to patients with non-small cell lung cancer, according to a study published in Nature Medicine.
“The findings from this study will help us identify and design better blood-based biomarkers in immuno-oncology,” said Young Kwang Chae, MD, MPH, MBA, associate professor of Medicine in the Division of Hematology and Oncology and a co-author of the study.
Atezolizumab monotherapy, an immune checkpoint therapy, is an effective treatment for patients with locally advanced or metastatic non-small cell lung cancer (NSCLC) whose tumors have high programmed death ligand 1 (PD-L1) expression. When PD-L1 is bound to the exterior of a cell, it tells roaming T-cells to leave the cell alone. Many cancers have upregulated PD-L1 to help hide cancer cells from the immune system.
However, a biopsy is required to determine PD-L1 levels and as many as 30% of patients with NSCLC may not have enough high-quality tissue biopsied at diagnosis for accurate biomarker analyses, according to Chae.
“We often run into the issue of insufficient tissue samples to run biomarker analysis in lung cancer, so it is important to develop a blood-based biomarker predicting response to immunotherapy,” said Chae, who is also a member of the Robert H. Lurie Comprehensive Cancer Center of Northwestern University.
In the trial, which enrolled 153 patients with NSCLC, investigators analyzed circulating tumor DNA (ctDNA) for tumor mutational burden (TMB), a measure of total mutations found in the DNA of cancer cells. Cancers with high TMB have been associated with a positive response to immune checkpoint inhibitor therapies.
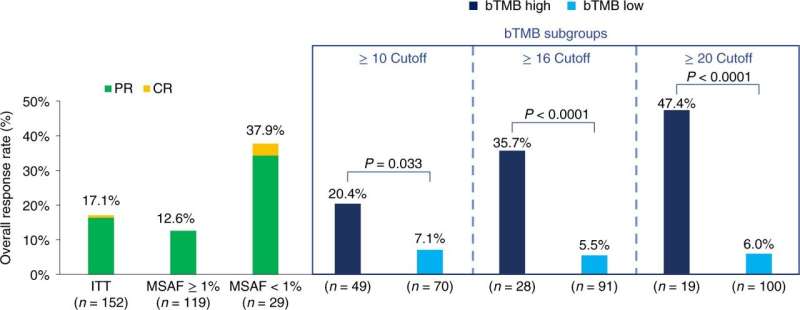
Of the patients, 28 had high TMB values—making them suitable for atezolizumab monotherapy—while 91 patients had low TMB values. Notably, the high TMB group was slightly younger and had more smokers.
All patients received atezolizumab monotherapy, and response rates to the therapy were much higher in the high TMB group—35.7% compared to just 5.5% in the low TMB group. Patients in the high TMB group also experienced longer survival than those in the low TMB group.
The findings demonstrate that measuring TMB in ctDNA is a viable option for stratifying patients for immune checkpoint inhibitor therapy, according to the authors. While more work is required to understand the relationship between TMB and immune checkpoint inhibitor therapy—hopefully revealing a sub-population of patients who would benefit most from the therapy—the foundations for therapy selection using a simple blood test are strong, according to Chae.
Source: Read Full Article
