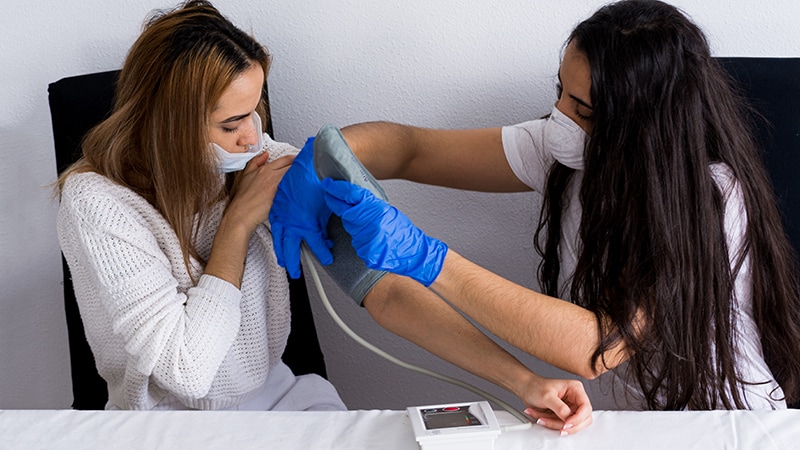
A Medicare plan to increase a 20-year-old metric used in setting payments for clinical labor, such as employment of nurses, drew praise. But there also are persisting concerns among groups slated for reductions to cover this new expense.
In the physician fee schedule for the current year, Medicare officials noted that clinical labor rates had last been updated in 2002 using Bureau of Labor Statistics (BLS) data and other supplementary sources where BLS data were not available. That was one of the reasons the Centers for Medicare & Medicaid Services (CMS) finalized the clinical labor rate changes for 2022 despite many objections.
This change is a win for family practice and internal medicine practices, CMS said in the final version of the rule, unveiled last year. CMS said the change in the clinical labor rate could increase access to care for disadvantaged groups such as women and racial minorities. Although members of specialties such as radiation oncology objected to the clinical labor rate increase because of the offset costs, other groups defended it.
In a December article in STAT, Sterling N. Ransone Jr, MD, president of the American Academy of Family Physicians (AAFP), said Medicare payments for registered nurses employed in practices had not reflected recent pay increases in this field, adding to financial strain on practices. Under the 2022 physician fee schedule, Medicare’s hourly rate for employment of registered nurses would rise from a rate of $30.60 to $51.
The bump in the clinical labor rate comes amid reports of intense competition for nursing staff. Medscape has reported that hospitals are trying to entice workers from other facilities to fulfill needs. A South Dakota health system was said to have offered signing bonuses up to $40,000 for experienced nurses who would make a 2-year commitment. Job listings for nurses in Maine and Virginia showed $20,000 signing bonuses.
In an interview, Ada Stewart, MD, AAFP’s board chair, spoke about facing challenges in her own Columbia, South Carolina-based primary care group to recruit and retain nurses.
“Right now they can go somewhere else and make so much more money,” Stewart said. “It was a big issue even before the pandemic but was worse with the pandemic.”
“This is something that’s been long overdue,” Stewart said about the clinical labor rate increase.
In a statement to Medscape Medical News, the American Nurses Association noted that the increase planned for 2022 is in payments made to practices that employ nurses, and not in pay directly to them. Registered nurses are not paid directly under Medicare, rather the clinical labor pricing is part of what a clinician, such as an advanced practice registered nurse (APRN) or a physician, is paid based on the service billed.
ANA said it “supports CMS examining payment reform to properly value the nurse for the work performed in all healthcare settings.”
Winners and Losers
Seeking to keep Medicare spending in check, Congress require CMS to often make cuts to offset increased spending in the physician fee schedule. The “budget neutral” requirement means clinicians in some specialties often stand to see their pay cut or shaved to accommodate increases for others.
In a statement to Medscape, Claire Ernst, JD, director of government affairs for the Medical Group Management Association (MGMA) noted the challenges involved with the increase in pay for nurses employed at practices.
“MGMA agrees that an update to the clinical labor pricing is reasonable, since it has not been updated in about 20 years. Due to budget neutrality requirements, any payment policy changes made to the physician fee schedule should be carefully evaluated as to not trigger significant cuts to certain specialties,” Ernst said.
“As we discuss the unintended consequences of fee schedule payment updates stemming from budget neutrality, the larger question of broader reform remains,” Ernst added.
CMS last year received many comments from physicians opposed to the planned bump in clinical labor rates because of the effect it would have on their practice. Physicians in specialties with high capital cost services, such as radiation oncology, for example, suggested that the offset costs should be spread equitably among all physicians and not borne disproportionately by those whose fields require significant investment in equipment.
Kerry Dooley Young is a freelance journalist based in Miami Beach, Florida. She is the core topic leader on patient safety issues for the Association of Health Care Journalists. Young earlier covered health policy and the federal budget for Congressional Quarterly/CQ Roll Call and the pharmaceutical industry and the Food and Drug Administration for Bloomberg. Follow her on Twitter at @kdooleyyoung.
Source: Read Full Article